Robotic Surgery
Science fiction is quickly becoming fact: robots can now perform surgery on humans.

Steven Spielberg once said, “There is no such thing as science fiction, only science eventually.” In this era of fast-paced technological advances and ever-growing human innovation, the time between science fiction and science is shorter than ever. One field that has truly seen the tremendous impact of these rapid advances is surgery, and more so, the field of robotic surgery.
What is Robotic Surgery?
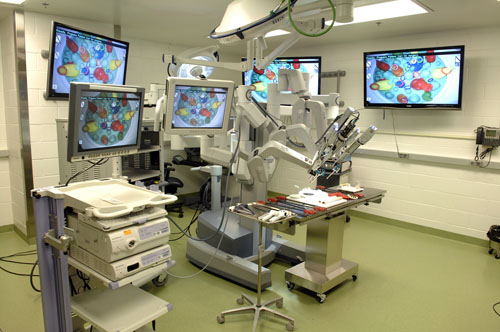
Robotic surgery is the use of robotics, high-definition imaging, computer-assisted simulation, and modeling for surgical procedures. It is performed in specially designed operating rooms (OR) equipped with a patient-side robotic cart, surgeon-side robotic console and various high-definition monitors.
Surgeons perform robotic surgical procedures on a specialized console, which provides a high quality three-dimensional image of the patient’s body. The surgeon controls the robot by maneuvering levers, pedals and buttons on the console with his arms, feet, fingers and wrists. The robot executes these commands through instruments attached to robotic arms on the patient-side robotic cart. Depending on the surgeon’s requirements, the instruments can be changed easily by a scrub nurse.
Should any errors occur during the surgery, robotic systems are constructed to be fault-tolerant. One built-in safety feature is called “graceful degradation.” If one component begins to fail, the system slowly compensates or degrades to a lower level of performance rather than suddenly quitting or causing an erratic motion. In such a case, the system permits the surgeon to take over and complete the procedure with conventional surgical techniques.
Pros and Cons
Compared to traditional surgery, robotic surgery provides a myriad of benefits to the surgeon as well as the patient. The patient undergoes less trauma and blood loss during surgery, which means there is less post-operative pain, a shorter hospital stay, and a faster recovery due to reduced scarring and improved healing of surgical wounds. Additionally, there is a reduced risk of infection for patients of robotic surgery.
“The main drawback lies in the cost of the robotic system, a roughly $1.2 million expense.
Overall, the robotic system augments the dexterity, precision and technique of the surgeon, thus making it possible for the surgeon to perform complex surgical procedures with greater ease. While executing the procedure, the robot reduces any erratic movements or tremors originating from the surgeon’s hand. This feature is particularly useful while performing surgeries where fine suturing is required. The surgeon-side console also provides a comfortable seated position for the surgeon that greatly reduces the fatigue during surgery. The surgeon also utilizes high-quality, live 3D images of the patient for a better perspective of the area to be operated on. The use of the robot also reduces the number of medical technicians needed in the OR, as the surgeon can control most parameters (e.g., camera position and angles) himself. Furthermore, working on the robotic console is highly intuitive, which measurably reduces the learning curve for training in surgery.
The main drawback lies in the cost of the robotic system. Current systems cost roughly $1.2 million, which is preventing many institutions from using robotic surgery.1 Furthermore, even though the use of the robot greatly reduces the intra-operative time in most procedures, it takes a considerable amount of time to set up the robot before surgery.
How It All Began
Surgical robotics has greatly evolved since it first came into existence in 1985 with the Puma 560, a robot used to perform neurosurgical biopsies with greater precision. This system eventually led to the development of PROBOT, a robot designed specifically for transurethral resection of the prostate.
In 1992, the FDA approved a new surgical robot, ROBODOC, for the first time in its history. ROBODOC was designed to mill out precise fittings in the femur for hip replacement surgery. By this time, surgeons had begun to accept the increased precision robotics could bring into surgery.2
In 1999, Intuitive Surgical Inc. further developed robotic systems with the introduction of the da Vinci Surgical System. While initial work was funded by the U.S. Army in the interest of developing a remote battlefield surgical system, possible commercial applications were even more attractive since this technology could be used to promote the practice of minimally invasive surgery.3
Robotic Surgery Today
The da Vinci Si system, a sequel to the da Vinci system, is the most commonly used robotic system for surgery. The system is FDA approved for a variety of surgical procedures, including those that are urologic, gynecologic, and thoracoscopic. Placed in over 800 hospitals and academic institutions in the United States and Europe, the da Vinci System was used in over 48,000 procedures in 2006 alone. The da Vinci prostatectomy procedure is currently the fastest-growing treatment for prostate cancer, which is the second leading cause of cancer-related death in men. 3
Surgeons with wide-ranging levels of expertise (from novice to expert) are now taking advantage of the da Vinci System in learning, performing, and teaching challenging surgical procedures.
What Improvements Can Be Made?
“Haptics is a new area of research that allows surgeons to feel force-feeback.
The field of robotic surgery is still in its infancy. Haptics is a new area of robotic surgery that allows surgeons to have a realistic sense of touch through the robotic systems by incorporating force-feedback.4 Force-feedback mimics the pressure that is felt in the fingers, hands and arms when manipulating an actual instrument. With it, delicate sensations on the pads of the fingertips and palms of the hands convey the subtle forces that can distinguish texture and traction. Such innovative enhancements to robot technology will greatly enhance the capabilities of human surgeons in the next few years.
The Operating Room of the Future
Professor Pier Cristoforo Giulianotti, a world-renowned robotic surgeon, is one of leading thinkers creating tomorrow’s operating rooms.1 Giulianotti’s vision of the future OR hinges on automation: a patient would be brought to a preoperative holding area on a smart stretcher, which would record vital signs and then anesthetize the patient. The nano-scale imaging devices installed in this smart stretcher would perform a total body scan, providing all vital diagnostic information about the patient.
Upon being prepared for a sterile environment, the patient would then be brought into the operating room. The smart stretcher would dock with the patient-side robotic console and would share the patient’s information with the surgeon’s console. An automatic tool changer would play the role of a scrub nurse while an automatic parts dispenser would act as a circulating nurse. The robotic surgery system would be similar to the one described above, except that sutures and gauze would be automatically dispensed. When a disposable (i.e., a supply or instrument) is used, the patient would be billed automatically, a new disposable would be restocked, and a request to reorder the disposable would be sent to the appropriate vendor.
This integrated operating room based on robotic and information systems would enable the surgeon to monitor every motion of the robot, providing a continuous quantitative record for quality assurance, error detection and reduction, post-operative analysis, and improved patient safety.
The system can also allow a surgeon to rehearse the patient’s operation on the patient-specific image before the actual surgery. Like a mission rehearsal in the military or a golfer practicing his swing before an important shot, the surgeon will be able to perfect the procedure or foresee potential complications by rehearsing many times before actual performance. The practice runs done on the patient’s image may also be recorded, precisely edited, corrected and then executed by the robotic system for an error-free procedure.
It may seem like science fiction right now, but this is truly going to be the reality of surgery in the future. With the current advances and tireless efforts of surgeons, engineers and biomedical researchers, such programmed surgeries would become a mainstream practice in the next decade.
Ethical Concerns
A natural issue that arises with robotic surgery is that of medical ethics. One of the key efforts made in this direction was the ETHICBOTS® European Project started in 2005. The aim of this three-year project was to bring together surgeons, philosophers, scientists and researchers from around the world to explore the “Techno-Ethical Issues in Bio-Robotics Technologies.”5
The conference was motivated by the fact that in the near future, robotic and intelligent information systems are expected to interact more closely with human beings. Though technology development is quickly producing information and robotic systems that are expected to enhance humans’ capabilities in significant ways, reflections on the ethical issues regarding bio-robotics and artificial intelligence lag far behind. Below are some of the pressing issues discussed at this conference.
Q. Would the use of robotics in surgery have a profound impact on the doctor-patient relationship? Would it compromise the human aspects of medicine?
A. As of now, the robotic system is only a tool used by surgeons to enhance their capabilities. The robot acts as a mere instrument, while the surgery is still performed by a qualified human surgeon who is present in the same OR as the patient. Also, pre-operative and post-operative care is still provided by doctors, nurses and other para-clinical staff.
Nevertheless, several remote surgeries have been performed in the past, and may certainly become more popular in the future because of convenience. 5 This could have an adverse impact on the doctor-patient relationship. To counter this problem, the use of telemedicine has been suggested. Telemedicine would allow the surgeon to interact with the patient, analyze reports and receive diagnostic information efficiently through high quality communication systems.
Q. If a complication occurs, will it be the fault of the robotic system or the surgeon?
A. In spite of the fault-tolerant features of the robotic system, errors and complications can occur. The medico-legal issues pertaining to the responsibility of a complication are still a gray area and an ongoing topic of debate. The developers claim that surgeons should continue to have greater responsibility, as they ultimately have control over a surgery. In case there is a conflict between what the surgeon wants to do and the safety constraints built into the robot, the surgeon can always override the constraints and force the robot to comply.
On the other hand, surgeons claim that even though the system has features such as “graceful degradation” and allows them to take over, complications occuring while the system is degrading should not be the responsibility of the surgeon.
No matter what the result of this debate, we must realize that technology can only compliment the surgeon; it can never replace the surgeon.
References
1Ballantyne, G. H., Giulianotti, P. C., & Marescaux, J. (2004). The Primer of Robotic and Telerobotic Surgery: A Basic Guide to Heart Disease. Philadelphia: Lippincott Williams & Wilkins.
2Meadows, M. (n.d.). Computer-Assisted Surgery: An Update. Retrieved April 6, 2009, from http://www.fda.gov/fdac/features/2005/405_computer.html
3 Intuitive Surgical – Hospital Resources. (n.d.). Retrieved April 5, 2009, from http://www.intuitivesurgical.com/hospitalresources/index.aspx
4Okamura, A. (n.d.). Johns Hopkins Robotics – LCSR. Retrieved April 5, 2009, from http://lcsr.jhu.edu/Main_Page
5ETHICBOTS Project. Emerging Technoethics of Human Interaction with Communication, Bionic, and Robotic Systems Coordination Action. Retrieved April 23 2009, from http://ethicbots.na.infn.it/index.php
6Marescaux J, Leroy J, Rubino F, Vix M, Simone M, Mutter D. Transcontinental Robot Assisted Remote Telesurgery: Feasibility and Potential Applications. Annals of Surgery 2002;235:487-92
Images courtesy of the Robotic Training Lab, Division of General, Minimally invasive and Robotic Surgery, University of Illinois, Chicago c/o Professor Pier Cristoforo Giulianotti et al.
1 comment
Interesting article and topic.