New App Will Help Lower Blood Pressure
Program uses the popular DASH diet

You might think that a cell phone could only drive blood pressure up, not down, but a team from the BU School of Medicine is studying a smartphone app they hope will lower high blood pressure by helping people control their weight.
“We got the idea of rebuilding the DASH diet using mobile technology,” says Devin Mann, until recently a MED associate professor of medicine and associate chief medical information officer for innovation and population health at Boston Medical Center.
The DASH (Dietary Approaches to Stopping Hypertension) diet, developed in 1992 by Thomas Moore, a MED professor of medicine and a Medical Campus associate provost, and a team of researchers from five academic institutions is designed to offer a healthy diet for the general public, and can offer an alternative to low doses of blood pressure medication. Supported by the National Heart, Lung, and Blood Institute, part of the National Institutes for Health, the DASH diet was judged the best diet plan six years in a row by U.S. News & World Report. Designed to lower blood pressure, it is also effective for weight reduction, lowering cholesterol, and managing or preventing diabetes.
In 2010, the University offered employees the free online DASH for Health Nutrition Program. In 2012, after attending a conference on mobile technology and health, Mann realized it was ripe for reinvention as a mobile app.
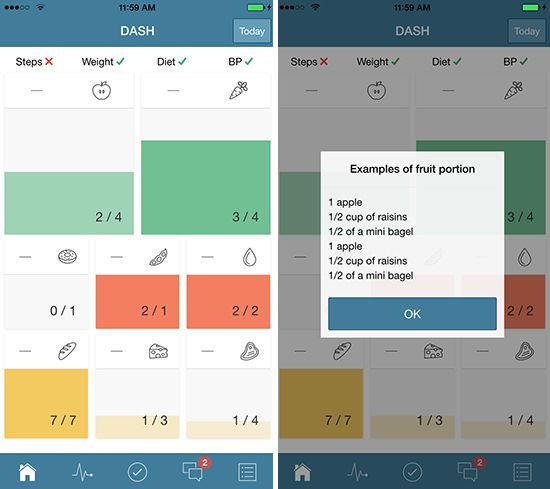
“Blood pressure is obviously a highly prevalent condition, and we thought [DASH] lent itself well to enhanced implementation with mobile health tools,” Mann says. “It’s truly evidence-based; it’s very clear cut what you need to do for it.” Participants in Mann’s study have their Android or iPhone equipped with the app, which asks users to record what they eat by tapping tiles that correspond to the eight components of a healthy diet. Bluetooth connects to a blood pressure machine, a scale, and a pedometer, all provided for the study.
Mann has departed his job for a position at New York University this month. He will still contribute, but the project will now be overseen by Lisa Quintiliani, a MED assistant professor of internal medicine and registered dietitian with expertise in behavioral science and medical informatics.
The simple food-recording interface “was a big piece of it, because diet tracking is one of the hardest things,” Mann says. Other apps “ask you to look up this food and the calories and all that stuff. We made a very conscious decision to say, listen, we will sacrifice accuracy for usability.”
The other key element of the smartphone approach is counseling. Some apps provide automated prompts based on data input. “We still feel human coaching is important, but setting up appointments is not easy to do,” Mann says. So the researchers enabled the app to connect study subjects with a dietician for twice-monthly 20-minute phone calls, during which counselors use motivational interviewing techniques originally developed for smoking cessation.
It’s important “having a counselor contact the participant to see where they are in terms of their readiness to change,” says Quintiliani. The counselors can then help the subject with goal setting and focus on areas where the subject is most ready.
“We’re using the app for all the things a computer is good for, and using a human for all the things a human is good for, which is listening and responding and building rapport,” she says.
Mann and others built an original version of the project a couple of years ago, after a seminar at Qualcomm got them “really excited about doing something with mobile applications,” Mann says. Last year, after a first attempt using undergraduate programmers fell by the wayside, they brought in BU Medical Center information technology staff and the Software & Application Innovation Lab (SAIL) at the Hariri Institute for Computing. An outside company, iHealth Labs, based in Mountain View, Calif., provides the Bluetooth-connected devices.
The MED team has recruited 24 participants for the study, which they hope to finish at the end of July, with analysis to follow. What happens next if the data supports the app’s effectiveness? A typical next step—quick commercialization—is not in the cards.
“I’m not sure that’s the right venue,” says Mann. The team’s vision is to use the app as a behavior modification module in a program overseen by a doctor. The doctor might say, for example, “You have pre-diabetes, here are six things I want you to do,” one of which is to sign up for the app and its coaching. Mann says he and his team want to figure out the most effective clinical approach to using the app before deciding how best to disseminate it.
“What we want to be able to say is that we’re confident in the approach, and then find the best way to scale that,” Mann says.
In the long run, they hope to develop a system that could be applied to change behavior for people with other health challenges. “It’s not really about blood pressure, it’s about the approach,” says Mann.
Comments & Discussion
Boston University moderates comments to facilitate an informed, substantive, civil conversation. Abusive, profane, self-promotional, misleading, incoherent or off-topic comments will be rejected. Moderators are staffed during regular business hours (EST) and can only accept comments written in English. Statistics or facts must include a citation or a link to the citation.