Taking Health Care High Tech
Terry Ellis uses mobile health technology to keep people with Parkinson's exercising

Photo by Steve Prue
It started in Denise’s thumb—a slight tremor when she gestured while talking. Just part of getting older, she thought. Or maybe it’s related to that shoulder problem I’m working out in rehab. Her rehabilitation therapist disagreed. “Go see your doctor,” she said.
Stephen’s handwriting tipped him off. It was getting smaller. Then there was that shaking in his left arm. His mother had experienced similar symptoms, and he knew what the doctor would say.
Denise and Stephen (last names withheld for privacy), both in their early 70s, are among an estimated 7 to 10 million people worldwide who have Parkinson’s, an incurable brain disorder that affects the nervous system, causing tremors, slow movement, stiffness, and impaired balance. Terry Ellis (MED’05), a Boston University assistant professor of physical therapy and athletic training and the director of BU Sargent College’s Center for Neurorehabilitation, is working to help patients with Parkinson’s like Stephen and Denise manage their disease through exercise.
Ellis’ research has shown that exercise can help patients improve their walking ability, strength, and flexibility, and may even slow the disease’s progression. But patients with Parkinson’s aren’t often referred to a physical therapist until years after their diagnosis, when function has begun to decline, Ellis says. Finding someone well versed in the disorder is difficult, especially in more rural areas, and patients’ engagement in exercise typically declines once therapy is over. Ellis and her colleague Nancy Latham, a research assistant professor in the Health & Disability Research Institute at BU’s School of Public Health, hope that keeping patients in touch with physical therapists through mobile health (mHealth) technology like smartphones and iPads will help.
“Especially with the explosion of aging populations, we’re going to have more and more people with these chronic diseases,” Ellis says. “So how are we going to help them maintain a high-quality life and the highest degree of function, and to be independent and age at home? I think physical therapy has a large role, but we need to think of new models of care.”
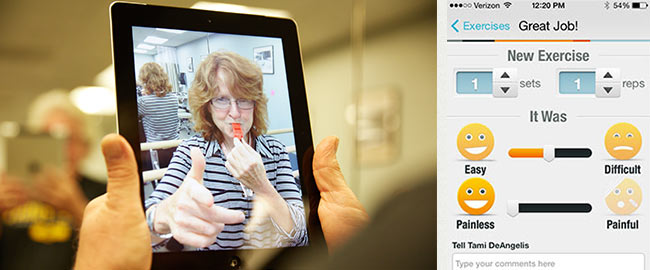
In fall 2013, with a $50,000 grant from the American Parkinson Disease Association, Ellis and Latham began recruiting for a pilot study featuring Wellpepper, application software designed to help patients stick to treatment plans. The participants, New England–area patients with Parkinson’s, are randomized into two groups: an mHealth group that uses Wellpepper on an iPad mini provided by Sargent and a control group that follows an exercise routine with the help of the traditional paper instructions and demonstrative photos. Participants in the mHealth group access personalized exercise videos—Sargent videotapes them performing prescribed exercises when they enter the program—and submit their daily progress and levels of difficulty and pain. They can also chat virtually with a Sargent physical therapist who receives their Wellpepper data and readings from pedometers linked to the app via Bluetooth wireless technology. Ellis chose the iPad mini based on focus group feedback, but ultimately would like to see the app available on any platform of the patient’s choice.
To participate in the program, Denise and Stephen traveled on separate occasions to the Center for Neurorehabilitation to meet with Tami DeAngelis (SAR’02), a senior physical therapist, who guided them through several exercises and gave them a pedometer and a daily walking goal. “I hope to get fitter,” says Stephen, who’s just starting out in the paper group, “and I hope it slows down the progression of the disease.” Denise, who has finished her six months in the mHealth group, says she is “willing to try anything, just so I don’t fall through the cracks.”
Patients appreciate the ongoing interaction and accountability mHealth technology offers, Ellis says. “They want the encouragement and some level of oversight—someone saying, ‘Hey, great job! Look how much you accomplished!’” The encouragement motivates Denise, who says mHealth technology keeps her on track with her exercise routine. She likes the personal interaction, as well as working with DeAngelis to switch up her program when she wants more of a challenge. DeAngelis checks Wellpepper regularly and says mHealth technology makes her feel more connected to her patients and better able to support them.
“Especially with the explosion of aging populations, we’re going to have more and more people with these chronic diseases. So how are we going to help them maintain a high-quality life?” —Terry Ellis
Data collection wrapped up in fall 2014, and preliminary study results are positive. When 18 participants had completed the first three months of the study, those using the iPad had a higher exercise adherence rate (81 percent) than those using paper (57 percent). They spent more time performing moderate-intensity exercise, reported more confidence in their ability to exercise successfully, and rated the program 9 out of 10 for satisfaction.
Sargent is ahead of the curve in experimenting with these technologies, which are examples of telehealth, the delivery of health services through electronic communications such as email, two-way video, and smartphones. As Ellis and Latham point out, telehealth’s possibilities are expanding as technology becomes a more integral and affordable part of people’s lives, and as health care professionals seek ways to counteract higher costs of in-person care and shorter lengths of stay in hospitals or rehabilitation facilities.
The Affordable Care Act, which includes provisions for telehealth, is giving the field a boost, says Karen Jacobs (SAR’79), a clinical professor of occupational therapy. Sargent has already incorporated telehealth into its occupational therapy curriculum, she says, and “is well-positioned to be a global leader in student training and faculty research” in the field. Participants in Sargent’s new Neurological Physical Therapy Residency Program, for example, are involved in observation and research for the Wellpepper project.
Telehealth poses challenging questions for the health industry: How will services be reimbursed? Will current licensing policies change to facilitate care across state and national boundaries? What steps will providers take to ensure patients’ privacy and the security of their information? But Ellis says now is the time for change. “We have to be innovative in coming up with new models of care to try to reach people. I think we can have a bigger impact than people realize.”