From Stem Cells to Lung Cells
Far-reaching implications for BU research

How do you grow stem cells into lungs? The question has puzzled scientists for years. First you need the right recipe, and it took BU researchers Darrell Kotton, Tyler Longmire, and Laertis Ikonomou seven years of trial and error and painstaking science to come up with it. “A lot had to happen to make a lung,” says Kotton. “It was a little more complicated than Julia Child’s ‘heat, eat, bon appetit.’”
Kotton is a School of Medicine associate professor of medicine and pathology and codirector of the Center for Regenerative Medicine (CReM), a collaborative effort between scientists at BU and Boston Medical Center that seeks to advance stem cell research and regenerative medicine. Longmire (MED’12) is a PhD candidate working at CReM, and Laertis Ikonomou is a MED assistant professor of medicine. Their research, published in today’s edition of the journal Cell Stem Cell, will likely have far-reaching implications in the study of inherited lung disease.
Scientists have been growing mature tissues from embryonic stem cells for years. Some tissues, like muscle and nerves, are relatively easy to grow, but others, including liver, lung, thyroid, and pancreas, have been much more difficult. These troublesome tissues all spring from the endoderm, the innermost layer of an early embryo. The endoderm forms when an embryo is about three weeks old and differentiates into organs as early as five weeks. Somehow, in these two weeks the endoderm transforms into differentiated organs as diverse as the lungs and the stomach. Kotton’s objective was to find the series of steps that takes the cells from endoderm to lung and then to purify the candidate lung progenitors, or ancestors, a goal that has eluded scientists until now. “The trick,” he says, “was in the engineering.”
Kotton’s key moment of inspiration came during a conversation in the hospital cafeteria. He had just started up his lab and was talking with colleague Wellington Cardoso, a MED professor of medicine and pathology, about how to generate lung tissue from stem cells. They mapped out a strategy, scribbling ideas on sheets of loose-leaf paper.
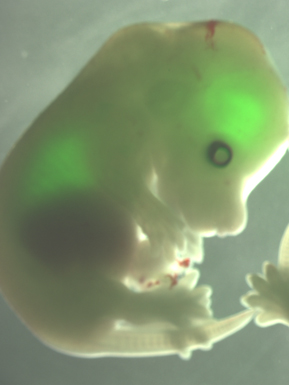
But something was missing. “We kept coming back to the idea of a reporter,” says Kotton. “Something that would be activated at the moment of specification.” He decided to create a knock-in reporter gene that would glow green during the “fate decision”—the moment when the stem cells expressed a gene called Nkx2-1 and thereby took a step toward becoming lungs. This allowed the team to track the cells as they developed, mapping each of the six critical decisions on the path to lung tissue. Kotton says the effort involved significant collaboration with other scientists, including Hans-Willem Snoeck of New York’s Mount Sinai Hospital and Jay Rajagopal of Massachusetts General Hospital, who helped at each step of the process.
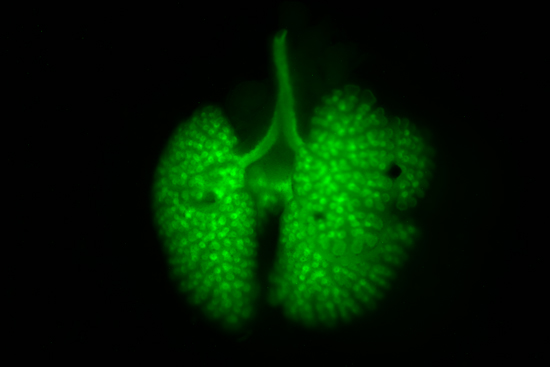
Once Kotton and his team had grown what appeared to be lung cells, they had to make sure they had the recipe right. They took samples of mouse lungs and rinsed them with detergent until they became cell-free lung-shaped scaffolds. They seeded one lung with 15-day-old homegrown lung cells that they had purified from stem cells. As a control, they seeded another lung with undifferentiated embryonic stem cells. Within 10 days after seeding, the lung cells organized themselves and populated the lung, creating a pattern recognizable to a pulmonologist as lung tissue. The stem cells in the control group grew and clumped into an unrecognizable mass.
A happy side effect of the discovery was that the scientists also mapped out the road from stem cell to thyroid. Thyroid, it turns out, also comes from the endoderm layer, deriving from a progenitor that expresses the same key gene as lung progenitors.
Kotton’s work will likely have a huge impact on lung stem cell researchers, who have been waiting for a discovery like this to propel their research on inherited lung disease. Stem cell research has held great promise since 2006, when scientists at the University of Kyoto first discovered how to take an adult differentiated cell, like a skin cell, and turn it back into a stem cell. These reprogrammed cells are called induced pluripotent stem cells, or iPS cells. In 2008, CReM codirector Gustavo Mostoslavsky, a MED assistant professor, streamlined the process by creating the stem cell cassette, or STEMCCA, a tool that allows scientists to easily reprogram adult skin cells into pluripotent stem cells. The tool, which BU patented, is now used worldwide and considered the industry standard.
Over the last few years, with this technology in hand, the CReM team collected skin cells from patients with various inherited lung diseases, such as cystic fibrosis and sickle cell anemia. Using the STEMCCA tool, they converted these skin cells into pluripotent stem cells, creating a disease bank with more than 100 lung disease–specific stem cell lines. Other researchers followed suit, but with no way to grow the stem cells into lungs, research stalled.
“All these researchers have stem cells sitting in their freezers waiting for a way to differentiate them into lung tissue,” says Kotton. “This opens up all those freezers.”
A note from the scientists at the Center for Regenerative Medicine, for people with further questions:
Thank you very much for your inquiries and interest in our work and potential stem cell therapies for lung disease. We caution all patients that stem-cell based therapies currently offered by several US clinics are experimental and not FDA approved, since they have not been rigorously tested in clinical trials for safety and efficacy. Patients considering such therapies for respiratory disease should consult the resources listed below before taking any decision.
The International Society for Stem Cell Research (ISSCR) offers excellent on-line resources for patients that consider stem cell-based treatments.
A statement on unproven stem cell interventions for respiratory diseases by the ATS Stem Cell Working Group
Statements by the Pulmonary Fibrosis Foundation, the Cystic Fibrosis Foundation, and the Alpha-1 Foundation regarding unproven/experimental stem cell interventions.
Comments & Discussion
Boston University moderates comments to facilitate an informed, substantive, civil conversation. Abusive, profane, self-promotional, misleading, incoherent or off-topic comments will be rejected. Moderators are staffed during regular business hours (EST) and can only accept comments written in English. Statistics or facts must include a citation or a link to the citation.