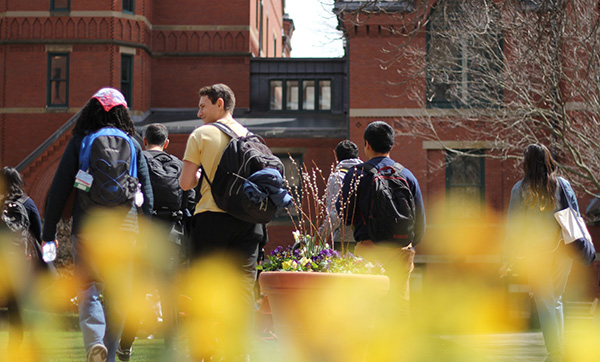Think. Teach. Do.
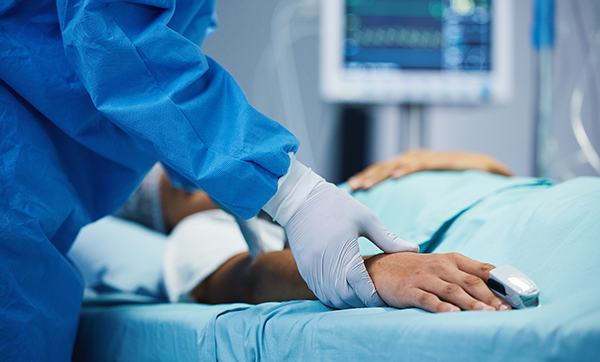
For the Health of All.
We educate the whole student. We help the whole world. If you’re seeking a graduate degree in public health, we probably share an ambitious goal—making a difference in the health and well-being of our global village. The question is: who can best prepare you to do so?
Top 10
School of Public Health according to U.S. News and World Report, ranked 8th in 2023
95%
of our students receive financial assistance
100%
of graduates employed or pursuing advanced education within 12 months of graduation.
150K+
people engaged in Public Health Conversations
Latest News
Upcoming Events
The Public Health Conversations event series bring speakers to our campus to engage in thoughtful conversations about the pressing issues of public health.

Wednesday, April 24, 2024
Artificial Intelligence and Health: Promise and Pitfalls
1:00-2:30 p.m. ET | Online

Wednesday, May 8, 2024
Nursing and The Health of the Public: The Next Decade
1:00-2:30 p.m. ET | Online


Wednesday, June 26, 2024
Teaching Public Health: Transforming Education for Public Health
9:00 am - 12:00 pm ET | In Person & Online
See yourself at SPH
As a top-ranked school of public health, our community offers you access to cutting-edge advancements in research, scholarship, and public health practice; a top-tier education with an on-the-ground mission.