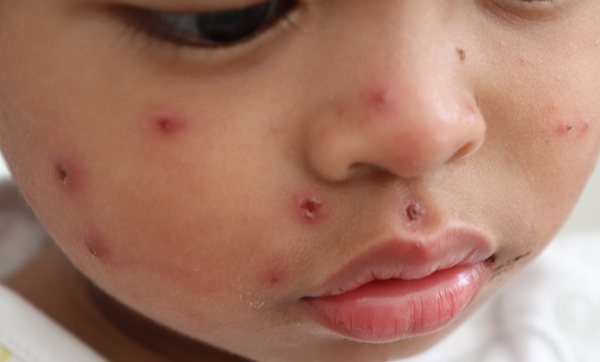
Global Health.
Mothers should survive childbirth so they and their babies can flourish.
People with diabetes should have access to life-saving insulin.
HIV-positive moms and dads should live to enjoy their grandchildren.
Global health has achieved dramatic reductions in preventable illness, injury and death. But there is still much to do. Our faculty, staff, and students are at the forefront of the global push towards the world’s Sustainable Development Goals--we are looking forward and acting now to eliminate poverty, inequity, and preventable illness and death by 2030.
Research
We collaborate with communities, governments, scientists, and international development partners to improve the health of populations.
Students & Alumni
We train future global health leaders through classroom and field-based experiences. DGH alumni are working around the world: improving government policies, promoting social justice, and increasing access to education, economic opportunity, and health services.
Partnerships
Over two decades we have built partnerships in Boston, China, Ghana, India, Mexico Vietnam, South Africa, Zambia, and elsewhere. These relationships drive our research, advocacy, and commitment to the communities where we work.
Global Health at a glance
Primary Faculty
Peer-Reviewed Articles Annually
Funding Agency Awards Annually
Affiliated Degree Programs
Affiliated Academic Programs
BU School of Public Health graduate degree programs providesstudents with specialized training in both the theory, research, and practice of global health.Students pursuing a Master's degree in Public Health (MPH) and have an interest in global health may choose to obtain a functional certificate learning to design and implement rigorous field-based projects and conducting monitoring activities in developing and developed countries. Doctoral in Public Health (DrPH) candidates learn to develop, implement, and evaluate national and global public health programs and policies.
MPH DRPH MS in Population Health Research Request Information Apply Now
Upcoming Events
April
Recent Department News
Recent media coverage
Global Health Latest Publications
- Published On 4/19/2024Reproductive and Social Policies, Sociopolitical Stress, and Implications for Maternal and Child Health Equity.Current environmental health reportsread at PubMed
- Published On 4/2/2024Disparities in Tuberculosis Incidence by Race and Ethnicity Among the U.S.-Born Population in the United States, 2011 to 2021 : An Analysis of National Disease Registry Data.Annals of internal medicineread at PubMed
- Published On 4/1/2024Future HIV epidemic trajectories in South Africa and projected long-term consequences of reductions in general population HIV testing: a mathematical modelling study.The Lancet. Public healthread at PubMed
- Published On 4/1/2024Estimating the health effects of COVID-19-related immunisation disruptions in 112 countries during 2020-30: a modelling study.The Lancet. Global healthread at PubMed
- Published On 4/1/2024Officer-Involved Killings of Unarmed Black People and Racial Disparities in Sleep Health.JAMA internal medicineread at PubMed